“Half of what we have taught you is wrong. Unfortunately, we don’t know which half.”
— attributed to a Harvard Medical School dean at commencement, sometime in the 20th century
The above, possibly apocryphal, statement is often invoked to illustrate how dynamic the field of medicine can be, and how what we thought we once knew beyond a shadow of a doubt, sometimes turns out to be dead wrong. It’s also a celebration of scientific progress; as we revise our pathophysiological models, we can develop more targeted therapeutics.
In this regard, psychiatry is no different from any other field of medicine. We don’t know (yet) what we don’t know, but once we do, our treatments will improve. At the same time, we need to be careful how we use this new information, lest it give us a false sense that we “know” something we don’t.
 I thought of this question when I encountered a headline earlier today at psychcentral.com: “How Lithium Works Finally Explained.” Talk about a tantalizing headline! First used clinically in the late 1800s (and later “rediscovered” in the 1940s), and still used extensively as a mood stabilizer in bipolar disorder and as adjunctive treatment for major depression, lithium is one of the most widely prescribed medications in all of medicine. Many patients report a very good response to lithium, and its efficacy has not been surpassed by the multitude of other mood stabilizing agents introduced in the last 40 years.
I thought of this question when I encountered a headline earlier today at psychcentral.com: “How Lithium Works Finally Explained.” Talk about a tantalizing headline! First used clinically in the late 1800s (and later “rediscovered” in the 1940s), and still used extensively as a mood stabilizer in bipolar disorder and as adjunctive treatment for major depression, lithium is one of the most widely prescribed medications in all of medicine. Many patients report a very good response to lithium, and its efficacy has not been surpassed by the multitude of other mood stabilizing agents introduced in the last 40 years.
But there’s just one problem. Nobody really knows how lithium works. It’s an ion (similar to sodium), so it doesn’t bind to a receptor or transporter, like most other psychiatric drugs. It doesn’t seem to affect membrane potential (and therefore neuron excitability), and it doesn’t seem to target any particular region of the brain, much less those thought to be involved in mood disorders. It may inhibit intracellular messengers (the phosphatidylinositol pathway) or it might inhibit cellular differentiation (via the Wnt signaling pathway). Maybe it blocks sodium ion transport. Maybe it interacts with nitric oxide. No one knows. And yet it works.
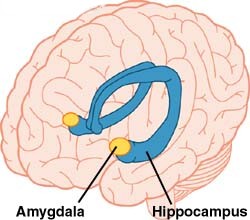 So it was with great interest that I read the original paper cited in the Psychcentral article. It’s a “mega-analysis,” published in the February 15 issue of Biological Psychiatry, of 321 bipolar patients in 11 centers worldwide who underwent MRI scans and were compared to non-bipolar controls. Half of the bipolar patients were taking lithium. To summarize the results, patients taking lithium had larger hippocampal and amygdala volumes than those not taking lithium, and patients with a longer history of bipolar disorder had reduced cerebral volumes.
So it was with great interest that I read the original paper cited in the Psychcentral article. It’s a “mega-analysis,” published in the February 15 issue of Biological Psychiatry, of 321 bipolar patients in 11 centers worldwide who underwent MRI scans and were compared to non-bipolar controls. Half of the bipolar patients were taking lithium. To summarize the results, patients taking lithium had larger hippocampal and amygdala volumes than those not taking lithium, and patients with a longer history of bipolar disorder had reduced cerebral volumes.
The data, then, seem to be consistent with the idea of lithium as having a “trophic” effect—i.e., as a promoter of neuronal growth, at least in some brain structures. But that’s about all we can say. Whether this has anything to do with intracellular signaling or the Wnt pathway, or with any known nerve growth factors, is beyond the scope of this study.
So despite the exciting headline claiming to identify the “mechanism of lithium,” this is simply an observation, much like the observation about how antipsychotics may decrease brain volumes, about which I wrote last week. It suggests further research to understand lithium’s effect on these regions. But it may not be clinically relevant.
Lithium is a widely used drug because it works. Period. These new data add to our knowledge about bipolar disorder, but to assume that they help us understand bipolar patients any better than we did before, is incorrect. Moreover, it may lead us to draw false conclusions about our patients (i.e., “he’s not responding to lithium so his hippocampus must be atrophied”) or, worse, reject or disregard data that don’t fit with our hypothesis. I’d much rather prescribe a drug because I have years of experience using it, and have heard hundreds of patients endorse its benefit, rather than adhere to an incorrect theory, even a theory with “face validity” like lithium promoting nerve cell growth and differentiation. In fact it’s not too hard to find arguments against this theory: for starters, consider lithium’s teratogenic effects during human embryonic development.
 Anyone who wants an accurate explanation for how a psychiatric drug works is, unfortunately, out of luck. The serotonin hypothesis is a perfect example: SSRIs work in a lot of patients, and the serotonin hypothesis helps to guide treatment, but it might be absolutely incorrect. How many alternate explanations have we ignored because we want to believe that our model must be right?
Anyone who wants an accurate explanation for how a psychiatric drug works is, unfortunately, out of luck. The serotonin hypothesis is a perfect example: SSRIs work in a lot of patients, and the serotonin hypothesis helps to guide treatment, but it might be absolutely incorrect. How many alternate explanations have we ignored because we want to believe that our model must be right?
We can, and should, continue to use SSRIs to treat depression, and lithium to treat bipolar disorder. But we should be aware that our explanations of their mechanisms are mere hypotheses—nothing more. And, moreover, that these hypotheses may be contradicted or proven wrong. Because we don’t know which half of our knowledge is the correct half.



 Posted by stevebMD
Posted by stevebMD 