 Are atypical antipsychotics overprescibed? This question was raised in a recent article on the Al Jazeera English website, and has been debated back and forth for quite some time on various blogs, including this one. Not surprisingly, their conclusion was that, yes, these medications are indeed overused—and, moreover, that the pharmaceutical industry is responsible for getting patients “hooked” on these drugs via inappropriate advertising and off-label promotion of these agents.
Are atypical antipsychotics overprescibed? This question was raised in a recent article on the Al Jazeera English website, and has been debated back and forth for quite some time on various blogs, including this one. Not surprisingly, their conclusion was that, yes, these medications are indeed overused—and, moreover, that the pharmaceutical industry is responsible for getting patients “hooked” on these drugs via inappropriate advertising and off-label promotion of these agents.
However, I don’t know if this is an entirely fair characterization.
First of all, let’s just be up front with what should be obvious. Pharmaceutical companies are businesses. They’re not interested in human health or disease, except insofar as they can exploit people’s fears of disease (sometimes legitimately, sometimes not) to make money. Anyone who believes that a publicly traded drugmaker might forego their bottom line to treat malaria in Africa “because it’s the right thing to do” is sorely mistaken. The mission of companies like AstraZeneca, Pfizer, and BMS is to get doctors to prescribe as much Seroquel, Geodon, and Abilify (respectively) as possible. Period.
 In reality, pharmaceutical company revenues would be zero if doctors (OK, and nurse practitioners and—at least in some states—psychologists) didn’t prescribe their drugs. So it’s doctors who have made antipsychotics one of the most prescribed classes of drugs in America, not the drug companies. Why is this? Has there been an epidemic of schizophrenia? (NB: most cases of schizophrenia do not fully respond to these drugs.) Are we particularly susceptible to drug marketing? Do we believe in the clear and indisputable efficacy of these drugs in the many psychiatric conditions for which they’ve been approved (and those for which they haven’t)?
In reality, pharmaceutical company revenues would be zero if doctors (OK, and nurse practitioners and—at least in some states—psychologists) didn’t prescribe their drugs. So it’s doctors who have made antipsychotics one of the most prescribed classes of drugs in America, not the drug companies. Why is this? Has there been an epidemic of schizophrenia? (NB: most cases of schizophrenia do not fully respond to these drugs.) Are we particularly susceptible to drug marketing? Do we believe in the clear and indisputable efficacy of these drugs in the many psychiatric conditions for which they’ve been approved (and those for which they haven’t)?
No, I like to think of it instead as our collective failure to appreciate that patients are more resilient and adaptive than we give them credit for, not to mention our infatuation with the concept of biological psychiatry. In fact, much of what we attribute to our drugs may in fact be the result of something else entirely.
For an example of what I mean, take a look at the following figure:

This figure has nothing to do with psychiatry. It shows the average body temperature of two groups of patients with fever—one who received intravenous Tylenol, and the other who received an intravenous placebo. As you can easily see, Tylenol cut the fever short by a good 30-60 minutes. But both groups of patients eventually reestablished a normal body temperature.
 This is a concept called homeostasis. It’s the innate ability of a living creature to keep things constant. When you have a fever, you naturally perspire to give off heat. When you have an infection, you naturally mobilize your immune system to fight it. (BTW, prescribing antibiotics for viral respiratory infections is wasteful: the illness resolves itself “naturally” but the use of a drug leads us to believe that the drug is responsible.) When you’re sad and hopeless, lethargic and fatigued, you naturally engage in activities to pull yourself out of this “rut.” All too often, when we doctors see these symptoms, we jump at a diagnosis and a treatment, neglecting the very real human capacity—evolutionarily programmed!!—to naturally overcome these transient blows to our psychological stability and well-being.
This is a concept called homeostasis. It’s the innate ability of a living creature to keep things constant. When you have a fever, you naturally perspire to give off heat. When you have an infection, you naturally mobilize your immune system to fight it. (BTW, prescribing antibiotics for viral respiratory infections is wasteful: the illness resolves itself “naturally” but the use of a drug leads us to believe that the drug is responsible.) When you’re sad and hopeless, lethargic and fatigued, you naturally engage in activities to pull yourself out of this “rut.” All too often, when we doctors see these symptoms, we jump at a diagnosis and a treatment, neglecting the very real human capacity—evolutionarily programmed!!—to naturally overcome these transient blows to our psychological stability and well-being.
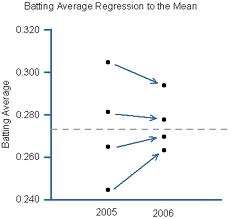
There’s another concept—this one from statistics—that we often fail to recognize. It’s called “regression to the mean.” If I survey a large number of people on some state of their psychological function (such as mood, or irritability, or distractibility, or anxiety, etc), those with an extreme score on their first evaluation will most likely have a more “normal” score on their next evaluation, and vice versa, even in the absence of any intervention. In other words, if you’re having a particularly bad day today, you’re more likely to be having a better day the next time I see you.
 This is perhaps the best argument for why it takes multiple sessions with a patient—or, at the very least, a very thorough psychiatric history—to make a confident psychiatric diagnosis and to follow response to treatment. Symptoms—especially mild ones—come and go. But in our rush to judgment (not to mention the pressures of modern medicine to determine a diagnosis ASAP for billing purposes), endorsement of a few symptoms is often sufficient to justify the prescription of a drug.
This is perhaps the best argument for why it takes multiple sessions with a patient—or, at the very least, a very thorough psychiatric history—to make a confident psychiatric diagnosis and to follow response to treatment. Symptoms—especially mild ones—come and go. But in our rush to judgment (not to mention the pressures of modern medicine to determine a diagnosis ASAP for billing purposes), endorsement of a few symptoms is often sufficient to justify the prescription of a drug.
Homeostasis and regression to the mean are not the same. One is a biological process, one is due to natural, semi-random variation. But both of these concepts should be considered as explanations for our patients “getting better.” When these changes occur in the context of taking a medication (particularly one like an atypical antipsychotic, with so many uses for multiple nonspecific diagnoses), we like to think the medication is doing the trick, when the clinical response may be due to something else altogether.
Al Jazeera was right: the pharmaceutical companies have done a fantastic job in placing atypical antipsychotics into every psychiatrist’s armamentarium. And yes, we use them, and people improve. The point, though, is that the two are sometimes not connected. Until and unless we find some way to recognize this—and figure out what really works—Big Pharma will continue smiling all the way to the bank.



 Posted by stevebMD
Posted by stevebMD 