de-lu-sion [dih-loo-zhuhn] Noun. 1. An idiosyncratic belief or impression that is firmly maintained despite being contradicted by what is generally accepted as reality, typically a symptom of mental disorder.
 The announcement this week of disciplinary action against three Harvard Medical School psychiatrists (which you can read about here and here and here and here) for violating that institution’s conflict-of-interest policy comes at a pivotal time for psychiatry. Or at least for my own perceptions of it.
The announcement this week of disciplinary action against three Harvard Medical School psychiatrists (which you can read about here and here and here and here) for violating that institution’s conflict-of-interest policy comes at a pivotal time for psychiatry. Or at least for my own perceptions of it.
As readers of this blog know, I can be cynical, critical, and skeptical about the medicine I practice on a daily basis. This arises from two biases that have defined my approach to medicine from Day One: (1) a respect for the patient’s point of view (which, in many ways, arose out of my own personal experiences), and (2) a need to see and understand the evidence (probably a consequence of my years of graduate work in basic molecular neuroscience before becoming a psychiatrist).
Surprisingly, I have found these attributes to be in short supply among many psychiatrists—even among the people we consider to be our leaders in the field. And Harvard’s action against Biederman, Spencer, and Wilens might unfortunately just be the tip of the iceberg.
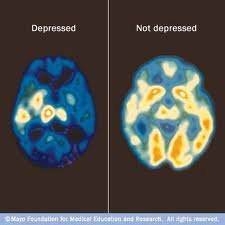 I entered medical school in the late 1990s. I recall one of my preclinical lectures at Cornell, in which the chairman of our psychiatry department, Jack Barchas, spoke with breathless enthusiasm about the future of psychiatry. He expounded passionately about how the coming era would bring deeper knowledge of the biological mechanisms of mental illness and new, safer, more effective medications that would vastly improve our patients’ lives.
I entered medical school in the late 1990s. I recall one of my preclinical lectures at Cornell, in which the chairman of our psychiatry department, Jack Barchas, spoke with breathless enthusiasm about the future of psychiatry. He expounded passionately about how the coming era would bring deeper knowledge of the biological mechanisms of mental illness and new, safer, more effective medications that would vastly improve our patients’ lives.
My other teachers and mentors were just as optimistic. The literature at the time was filled with studies of new pharmaceuticals (the atypical antipsychotics, primarily), molecular and neuroimaging discoveries, and novel research into genetic markers of illness. As a student, it was hard not to be caught up in the excitement of the coming revolution in biological psychiatry.
But I now wonder whether we may have been deluding ourselves. I have no reason to think that Dr Barchas was lying to us in that lecture at Cornell, but those who did the research about which he pontificated may not have been giving us the whole story. In fact, we’re now learning that those “revolutionary” new drugs were not quite as revolutionary as they appeared. Drug companies routinely hid negative results and designed their studies to make the new drugs appear more effective. They glossed over data about side effects, and frequently drug companies would ghostwrite books and articles that appeared to come from their (supposedly unbiased) academic colleagues.
This went on for a long time. And for all those years, these same academics taught the current generation of psychiatrists like me, and lectured widely (for pay, of course) to psychiatrists in the community.
 In my residency years in the mid-2000s, for instance, each one of my faculty members (with only one exception that I’m aware of) spoke for drug companies or was being paid to do research on drugs that we were actively prescribing in the clinic and on the wards. (I didn’t know this at the time, of course; I learned this afterward.) And this was undoubtedly the case in other top-tier academic centers throughout the country, having a trickle-down effect on the practice of psychiatry worldwide.
In my residency years in the mid-2000s, for instance, each one of my faculty members (with only one exception that I’m aware of) spoke for drug companies or was being paid to do research on drugs that we were actively prescribing in the clinic and on the wards. (I didn’t know this at the time, of course; I learned this afterward.) And this was undoubtedly the case in other top-tier academic centers throughout the country, having a trickle-down effect on the practice of psychiatry worldwide.
Now, there’s nothing wrong with academics doing research or being paid to do it. For me, the problem is that those two “pillars” by which I practice medicine (i.e., respect for the patient’s well-being, and a desire for hard evidence) were not the priorities of much of this clinical research. Patients weren’t always getting better with these new drugs (certainly not in the long run), and the data were finessed and refined in ways that embellished the main message. This was, of course, exacerbated by the big paychecks many of my academic mentors received. Money has a remarkable way of influencing what people say and how (and how often) they say it.
 But how is a student—or a practicing doc in the community who is several decades out of medical school—supposed to know this? In my opinion, those who teach medical students and psychiatry residents probably should not be on a pharma payroll or give promotional talks for drugs. These “academic leaders” are supposed to be fair, neutral, thoughtful authorities who make recommendations on patient outcomes data and nothing else. Isn’t that why we have academic medical centers in the first place? (Hey, at least we know that drug reps are paid handsome salaries & bonuses by drug companies… But don’t we expect university professors to be different?)
But how is a student—or a practicing doc in the community who is several decades out of medical school—supposed to know this? In my opinion, those who teach medical students and psychiatry residents probably should not be on a pharma payroll or give promotional talks for drugs. These “academic leaders” are supposed to be fair, neutral, thoughtful authorities who make recommendations on patient outcomes data and nothing else. Isn’t that why we have academic medical centers in the first place? (Hey, at least we know that drug reps are paid handsome salaries & bonuses by drug companies… But don’t we expect university professors to be different?)
Just as a series of little white lies can snowball into an enormous unintended deception, I’m afraid that the last 10-20 years of cumulative tainted messages (sometimes deliberate, sometimes not) about the “promises” of psychiatry have created a widespread shared delusion about what we can offer our patients. And if that’s too much of an exaggeration, then we might at least agree that our field now suffers a crisis of confidence in our leaders. As Daniel Carlat commented in a story about the Harvard action: “When I get on the phone now and talk to a colleague about a study… [I ask] ‘was this industry funded, and can we trust the study?'”
It may be too late to avoid irreparable damage to this field or our confidence in it. But at least some of this is coming to light. If nothing else, we’re taking a cue from our area of clinical expertise, and challenging the delusional thought processes that have driven our actions for many, many years.

That’s the #1 story at the Boston Globe. #2? Harvard docs at Mass General again are being investigated for not reporting adverse effects of a hip fx study – allowing some patients to suffer severe adverse effects – oh yeah – and 7 deaths. http://is.gd/E9hhBN
The head of Partners, the parent org over Mass General (and Brigham and Women’s) is a psychiatrist, Gary Gottlieb. His wife, Derri Shtasel, also a psychiatrist, is the Mass General director of community psychiatry. The psychiatry department there is extraordinarily invested (pardon the pun) in research – Popakostas, Fava, Mischoulon, Nierenberg et al rake it in around depression.
I think that Harvard and Mass General (and probably all of the Partners hospitals) need to have a full stop and time out to look at what the hades is going on.
I’m sorry you had the experience you did in medical school. It would be nice to be able to time warp and go back to pre-prozac days and chat a different course. But perhaps you will decide to lead another way through this muck!
Thank “God” (aka Biederman) that you had a solid scientific education before going into psychiatry. You mastered the tools to see the crap that masquerades for science in our intellectually, morally, but not economically (for the KOL’s who have been on the take for so many years) bankrupt profession . And you are a better psychiatrist for that training. Kudos!
Steve,
What you are witnessing is the death of your profession.
Psychiatry is dead.
Duane
P.S.: I’m not in the mood for any lectures on being ‘biased’…
Our son was caught up in Biederman’s bipolar juggernaut (overnight 40-fold increase in juvenile ‘bipolar disorder’)
The little deity ought to be in prison!
“each one of my faculty members (with only one exception that I’m aware of) spoke for drug companies or was being paid to do research on drugs that we were actively prescribing in the clinic and on the wards. (I didn’t know this at the time, of course; I learned this afterward.)”
I find it hard to believe that you really didn’t know that this was going on while you were a resident. When I was at the same institution a few years after you, even though that institution had banned pharm reps from being on campus, it was quite well known amongst all residents that most faculty members either did drug talks and/or got drug company funding for their clinical trials. Or maybe psychiatry residents have just become more skeptical of academic psychiatry over time?
Dr. D,
Thank you for that comment. You are correct that I “knew it was going on,” but only for a few faculty members who would make such arrangements known. In the years since, I have been surprised to learn the extent of some of their involvement with industry, and I never would have guessed the dollar amounts were as high as they are.
The real issue, though, is that many generations of residents and countless community physicians have listened to these academic “opinion leaders” without knowing that their opinions may not have been entirely their own. [My favorite examples were the Geodon and Abilify lectures I heard from two different professors during residency, which I later learned were from slides provided by Pfizer and BMS!]
Yes, times are changing, but so much of this stuff went on for so long, and as I’m sure you know, it’s hard to change doctors’ ways. Do I expect all psychiatrists to stop prescribing atypicals tomorrow? Of course not. In fact, I’m afraid that the most common response to the Harvard news (for the doctors that even hear about it) will be a yawn, a “what else is new,” and back to business as usual.
I don’t think anyone is yawning now. I do wonder what the tipping point will be, though.
Perhaps evidence-based medicine will come to the rescue because as non-pharma. interventions are demonstrated to have efficacy without iatrogenic physiologic derangements, such as that per permanent up/down receptor regulation, organized psychiatry might be motivated to move in that direction.
It’s ironic that you use the phrase, “business as usual”. Treatment as usual and business as usual are resulting in patient harm, and the outcomes are abysmal.
Perhaps a question for another post, but what do you envision as the preferred future or way forward?
Steve,
“back to business as usual”?
This is why your profession is dead.
Duane
Just to throw the cat among the pigeons, I’m going to put the blame for this problem on Harvard/other teaching facilities and the NIH (or NIMH). And because it’s not confined to psychiatry or even medicine, to the DOD, DOE, DOetc.
It seems that these institutions have/had employment contracts so lax that faculty members and/or those given grants to work on taxpayer-funded research projects were allowed free rein to enrich themselves with payments from drug/equipment/device companies.
Why was this allowed to happen? Why aren’t payments made by the drug companies given to the institutions first, and then parcelled out to the people who worked on the project or, heaven forbid, credited to the US taxpayer?
At least some light is now being thrown on these payments — and payments to Chuck Grassley and other Members of Congress, too, in the form of campaign contributions. Let’s hope the IRS is paying attention where appropriate.
As to what comes out of these studies/projects: I try to keep an open but critical mind, and try to read each paper on its merits and see how the information squares with what I’ve read in the past. And I’m not a Biederman hater — the last paper I read of his concluded that the drug didn’t work for the population in question.
The drug didn’t work because he didn’t get his check!
Good point.
A large enough check, and Biederman made things work!
A prostitute by any other name…
Duane
OMB, Tom, I never thought of that!
“Beidermania…” –
http://1boringoldman.com/index.php/2011/07/03/bipolar-kids-biedermania-and-super-angrygrouchycranky-irritability/
Duane
I practice psychiatry in a CMHC 20 hours per week, and if there’s one effect of biological psychiatry that doesn’t get enough attention is that it made the practice of psychiatry (and therefore the blogging of psychiatry) incredibly boring. I actually enjoy this blog, but not because it’s terribly interesting, but because I feel camaraderie with the host in many ways. The tone here is one of frustration, that I identify with. The Last Psychiatrist is the best psychiatry blog (and Thought Broadcast is also one of my new favorites), but his best posts are usually criticisms of psychiatry, criticisms of society, or Clinical Psychology–they’re not actually modern psychiatry. There is nothing interesting about actual practice, other than the surreal feeling I experience when the reality of what I’m expected to do strikes me. (Although I haven’t been accused of bigotry like our host, thankfully). Modern psychiatry is incredibly boring to discuss and to practice. I’m always amazed at how biological psychiatry could take something so inherently fascinating, and squeeze every drop of humanity and intellectual interest from it. Do people read biological psychiatry books just because they’re interesting? To learn about themselves? Their relationships with others? Psychiatry doesn’t even pretend to be interested in human behavior, motivation, or relationships. A psychopharmacologist must be one of the most boring professions in the world. I sometimes drink dozens of cups of coffee just to feel my heart ricocheting around in my chest cavity. Psychiatry has painted itself into a corner. Thanks for your efforts here.
Gary,
You can still do psychotherapy (although obviously not in a CMHC). You can do it a few hours a week and make more money the rest of the time. I don’t recommend doing psychotherapy all day long either – it’s too much work. Fascinating, but it requires enormous concentration if you’re doing it right. But don’t sign up with any managed care company that does not pay a reasonable amount for a 90807 code.
We’re a shortage specialty and they need us. Don’t let them try to tell you otherwise. Don’t be cornered in to being a bored script-writing machine.
If young psychiatrists would stand up for the full scope of practice, the field wouldn’t be in this mess.
When you say, “they need us” – who’s they? Are the candidates for psychotherapy at CMHCs triaged based on need? Or is it all based on $$?
How is it that treatment is determined not based on the best matched intervention to need, but based on provider whim?
If non-pharma interventions are deemed just, if not more, efficacious, lower risk and more acceptable to patients, why isn’t this a key clinical practice driver? Even if it’s not being reimbursed, why aren’t psychiatrists lobbying for it?
This seems to have been dumped onto the backs of already untreated, undertreated and mal-treated patients who are lacking the financial, political and influential clout to influence policy changes.
And of course, I’m asking rhetorically – not directing this fusillage at you, David.
2 thoughts:
1) You don’t know what you don’t know, and you don’t know what to ask if you don’t know. Steve and other reidents may well have known about the tip of the payment iceberg but not had the info to even think of the follow up questions as to how deeply entrenched in the money system were faculty, etc.
2) Media has certainly raised the level of awareness of the population as a whole to the issue of moneychangers from pharma to medical community, but as far as I can tell it is the entire medical system that is infused with this I’ll scratch your back, you scratch mine. After all, go to your GP and the probability is he will give you a script for whatever the pharma rep presented to him.
Carol
http://apainedlife.blogspot.com/
Carol,
“…may have known about the tip of the payment iceberg…” Yes, that is precisely the case. I’m not so naive to think that my teachers had no relationships with pharma, but I had no idea of the extent to which they were involved. I actually like Jackie‘s suggestion above that institutions (as opposed to individuals) should be the sole recipients of pharma money. $1 million to MGH goes a lot farther in advancing human health than $1 million to Biederman’s bank account. (Of course, if this were the case, a lot of bright young students wouldn’t choose psychiatry as a career.)
“go to your GP…” This reminds me of a patient I saw recently. It was her first time with a psychiatrist (and she had no psych or psych med history), but she had seen her GP a few weeks earlier and complained of feeling depressed. He prescribed Oleptro, Pristiq, and Lunesta (all at once, on the basis of a sole complaint), and asked her to let him know how she felt in 2 months. For those of you with any knowledge of psychiatric medications, this approach is laughable (and, most likely, dictated by the pharma rep or advertising, certainly not by data or experience), but it is, sadly, the way a lot of psychiatry is practiced in this country.
Steve, My mother had a long history of psych difficulties. Everytime she called her doctor to make a complaint about something her doctor said “take an extra pill.” (Re: disciplining: my mother knew about dogs and this doc would call my mother to ask for information about the doc’s dogs. I wrote the Pa. med. soc about this and that she was telling my mother to take all these extra pills, without seeing her in person. The response: be glad that she is so interested in your mother. No concern whatsoever about the level of care she was receiving.
Great post. This is an issue that has not received nearly enough attention. Fortunately, drug company funding and tweaking of cme is starting to come under closer scrutiny and regulation. However, residency education remains a wild west where anything goes and conflicts of interest run rampant. Faculty on the take often don’t realize the extent to which their own exposure to reps and speaker training sessions biases them, and the residents they teach don’t realize that many of the clinical “pearls” passed on by their attendings originated from the mouths of drug company reps. The attending who taught our second and third year psychopharm course was so shameless as to use drug company-produced slides in his lectures to us. He had our ears and our trust in the classroom and in the psych ER and, not surprisingly, we all emerged from it with a certainty that every depressive had a tinge of “bipolarity” and was an excellent candidate for Abilify. I later learned that this same attending was earning more than $100K annually from his drug company work (though certainly, his greatest value to the companies was as an educator of residents and maker of lifelong bipolar finders and Abilify devotees). In my current job, I work with a guy who probably doubles his salary by meeting with rural Kansas family practitioners and teaching them to recognize bipolarity (his version requires just one dsm criterion, occuring at any point in one’s life, for any duration, regardless of context) and lowering their inhibitions about prescribing “serious” psych drugs like Abilify and Lamictal. I often find myself a target of his pitches (“Have you thought about a little sprinkle of Abilify”) and have lost any desire to discuss challenging cases with him, as his conclusions (bipolar) and recommendations (Lamictal, Abilify or the newest product of whatever last rep had his ear). Just the other day, he was recalling how he told an FP resident rotating with us that “Lamictal will save your ass every time. And I regularly find myself having to counteract the misinformation he spreads among our local primary care community, who are now all too confidently prescribing Abilify and Lamictal for unapproved uses.
Great comment, Jeff. This reminds me of another recent patient, a 50-something man referred to me by his GP because of great difficulty with a taper off high-dose Klonopin. He indeed suffered significant withdrawal symptoms along with underlying anxiety (but had no significant psych hx before starting Klonopin). At the urging of his girlfriend, he went for an “evaluation” at the local academic med center. He had a ten (yes, 10!)-minute appt with a guy who is a well-known schizophrenia researcher. You can guess the diagnosis. Treatment recommendation? Seroquel.
If I were a nonpsychiatrist, I’d defer to the “expert” and give the Seroquel. Unfortunately, I’d be doing the patient a disservice as he was clearly suffering benzo withdrawal which (as you know) can be very difficult to treat.
(Of course, at the same time, Seroquel might have “helped”– which would, of course, vindicate the expert but also reinforce how screwed up psychiatric diagnosis really is.)
Re. the comments above by Dr. Steve and Jeff M:
When GPs/FPs/pediatricians/any physicians prescribe meds like in the scenarios you described — any kind of meds — without regard for the patient or the pharmacology of the meds in question, isn’t that straight out malpractice?
I’m thinking that the buck for malpractice stops at the doctor writing the scripts, no matter if s/he was influenced by pharma reps, a travelling huckster MD, etc.
Jackie,
You betcha!
Happy 4th of July to you, Dr. Allen — and to everyone reading.
Re: AEK’s reply to my reply to Gary’s post:
You are absolutely right on all points. The fact that organized psychiatry does not do nearly enough to truly advocate for the chronically mentally ill is scandalous.
I was referring to private insurance companies when I said “they” need us as much as we need them.
The fact that CMHC’s provide the bare minimum (and often highly inappropriate) psychopharm treatment and no psychotherapy at all is indeed all about money – taxpayer money.
The seriously mentally ill do not vote in large numbers, and the already dreadfully underfunded CMHC’s are taking even more of a hit in the bad economy. And the Republicans act like little Scientologists and imply that the chronically ill are all just faking it (although there are indeed some people who are in fact faking it to game the system).
So it’s not just psychiatrists who have to organize to solve this problem. Be careful who you vote for.
In my view, it’s not as easy as saying it’s a Republican vs. Democrat issue. Disregard of the mentally ill, and those in chronic pain and with other “invisible” health issues (like sleep problems), don’t get respect — or enough funding — under any administration.
Maybe it’s because the “communities” don’t make enough noise. Where is our Michael J. Fox? Who is our “face of …? I’d hate to see us fight along political lines because I think this transcends politics.
RE: “Advocacy”
IMO, the paradigm shift will not likely take place in psychiatry, or even psychology for that matter…
It will likely take place within the ‘rehabilitation’ community… Beginning with adherence to the “least restrictive” clause of the Americans with Disabilities Act (ADA).
Some good work is taking place at Boston University – Repository of Recovery Resources, along with Temple University – Collaboration on Community Integration.
From the National Council on Disability –
Click to access ncdreportexecsummary.pdf
Duane Sherry, M.S., CRC-R
http://discoverandrecover.wordpress.com/freedom
Or how about the “patient” community? There’s a novel concept.
The “recovery” movement is a ‘patient’ community in many ways… although many are ‘former patients’….
Some are on psychiatric drugs, others not…
Some involved in drug withdrawal, others are not interested. Some are fully-recovered, working… Others are in the process.
Lots of different kinds of folks.
It’s not a one-size-fits all movement.
Each person involved gets to talk for themselves.
Freedom (not ‘forced treatment’) the common denominator.
Duane
Jackie,
The pdf from the National Council on Disability (above) is titled, ‘From Priveleges to Rights: People Labeled with Psychiatric Disabilities Speak for Themselves’.
Emphasis, on “speak for themselves.’
Duane
For a quick moment it seemed Patty Duke might be, coming forward about her lifelong struggle with bipolar disorder. One of the problems seems to be you have to be there at the exact right moment.
Like it or not there will always be a segment of the population with psychiatric disorders who are not able to speak for themselves. Those people must not be ignored in your fight to see the death of psychiatry. (I think Duane, that was your term (or words)
Those who are unable are the easiest to disregard and throw away.
Have to advocate again for chronic pain patients as well as the seriously mentally ill to whom David Allen refers. Neither group have the ability to organize and go to Washington and make their faces, as well as voices, known. Because of that it is too easy for the moneydeciders and politicians to shrug their shoulders and say “who (or why) cares” or worse.
You cannot ignore what happened in NYC when they emptied out the hospitals and let the former patients fend for themselves. Some could not and became homeless and caused tremendous distress to themselves as well as the community. Theory is nice but actuality isn’t always.
Last comment on this topic. Steve, I hope I haven’t hogged the board… If so, apologize, but I would like to say a few things quickly….
Carol,
It’s more than “theory”… Recovery is taking place in lots of ways, in lots of places (although not nearly enough)….
Recovery from even the most severe forms of “mental illness” was commonplace back in the mid-1880s…. A collection of research studies done as far back as the 1970s showed that the majority of people recover from ‘schizoprenia’. (See National Empowerment Center).
So emptying the psychiatric hospitals (as was done by then President Ronald Reagan) was a compassionate thing to do.
The problem was that the lock-ups (done for years) was not replaced by a safe place to stay, and empathy… They were instead replaced by a ‘medical model’ of care; an ‘illness management model’… A lifetime of drugs for people with ‘severe mental illness’… And this model has been as much a failure as the institutional model for the vast majority of people.
Dr. Allen,
Re: Republicans not understanding or caring about the “mentally ill”… I suppose the Forbes family never got the memo…
They put their own private money into the Freedom Center in Massachussets –
http://www.freedom-center.org/
The Freedom Center was co-founded by a Will Hall, who was himself diagnosed with ‘schizophrenia’… He’s doing a lot of good for the people of his state, while he enjoys his own ‘recovery’.
Steve,
I didn’t mean to get into politics, but it was brought up by Dr. Allen, and I thought it unfair of him to paint an entire political party in the way that he did.
I think both parties have been at fault for receiving money from the pharma lobby, and for continuing down this path of failure with the current paradigm.
Re: Recovery
We can do better.
We HAVE to do better.
Duane Sherry, M.S.
http://discoverandrecover.wordpress.com
I was at Columbia P&S in the mid-80’s when DSM-III had been entered into the canon of holy books. A preceptor of mine, Michael First, was working on D-Tree, a desk-top interface meant to make psyche diagnoses from questions based on the DSM-III template.
In retrospect, this was the nadir of academic psychiatry. I hope that you, Steve, and like-minded colleagues will restore psychiatry to its roots, and will abandon the biological fallacy once and for all.
And I hope the opposite.
To the commenter who knows the Kansas doc look him up in the Dollars for Docs database http://projects.propublica.org/docdollars/ The database is by ProPublica and Biederman’s friends http://projects.propublica.org/docdollars/search?term=thomas+spencer&state%5Bid%5D= STILL took money after Grassley began the inquiry.
They did not make a ‘mistake’ they were caught and it’s that simple, the letter Mea Culpa is part of PR and the hand slap these men received is par for the course, until the Government grows a pair and stops allowing the health industry to be ran by corporations.
There are drug paradigms in place as ‘standard’ practice of care and treatment for childhood bipolar because that is how the KOLs and Pharma intended it.
Don’t forget the PAXIL 329 study where they signed off to have it appear favorable for GSK in treatment of teens, and they KNEW it caused suicidal thinking. Just like AstraZeneca KNEW as did Lilly that Seroquel and Zyprexa caused diabetes and weight gain, these companies are in it for P R O F I T and the paid doctors taking income like Biederman et al are nothing short of being called pharma pimps. Nemeroff included and not forgotten for how Bernard Carroll described him once as “so toxic he glows in the dark”.
Check out Boring Old Man blog for the Biederman series, it’s the truth, based on facts and it’s what this is all about, it’s what happened to my child, she’s a product of an industry gone out of control, a diagnosis that became a freight train with a one way ticket to disaster, there will be no turning back to regain the lost youth of America, until people STOP and research and learn how this all came to be, then take a look at the recent articles of illegal marketing fines by the Dept of Justice for most of the psychiatric meds, such as Trileptal, Risperdal, Zyprexa, Seroquel, Lexapro, the list goes on and on –these drugs were marketed with you and the kids in mind! This is why the drugs aren’t working if you wondered, it’s why the Institutions are still full of “sick people” it’s why people are on (via Whitaker’s book) record numbers of disability for psych dx and on boatloads of drugs NOT functioning in the world.
This is a reminder (the Biederman scandal revisited from 3 years ago) that this is going on, it never stopped and there are no plans to stop it.
AstraZeneca just recently had to post as part of a multistate litigation lawsuit all doctors paid by them. Have you seen the list? it’s incredible! it’s on their site as a reprimand, yet the doctors hands are out, waiting for the big bucks. Does that make your doctor a bad guy if he pockets 50K or 100K a year from pharma? That’s for you to decide. Does he offer you the meds his company he represents in talks sells> because that’s a conflict of interest you should know about.
Great post, Steve, and thanks for the link too.
Of everything you said, I must say the title of your post resonates the most. In the last few years I have rapidly come to the conclusion that seemingly everything we thought we knew (and thought to be effective) in this country (whether it be economic models, higher education/student loans, psychiatry, or health care in general) isn’t working anymore or was an all-out snow job by insatiably greedy corporate elites. The breadth and depth of the corruption is downright vertiginous. And it’s spiritually, mentally, physically, and emotionally exhausting to endure. I wouldn’t be surprised if we have to re-evaluate nearly all our most-cherished values in the next decade or face cultural, social, medical, and economic ruin like never before in this country. It could spell the end of an empire if we don’t.
I’d just like to say I’m no novice in the arena of psychiatric corruption. I was put on Paxil at age 14 for what was, in hindsight, perfectly understandable situational anxiety over my dad’s cancer diagnosis that I’m certain would have remitted naturally with talk therapy. And here I am, 13 years later, still on an SSRI (Lexapro) because no psychiatrist knew how to withdraw me from the medication without me having unbearable withdrawal symptoms. And now the long-term symptoms have set in, which are devastating: sexual dysfunction (ED, low libido, reduced pleasure in orgasm), and emotional anhedonia and lack of motivation, which gives me odd and pervasive social anxiety I NEVER used to have. All these symptoms cost me my first romantic relationship.
I am currently tapering my Lexapro very slowly and will hopefully be off next year, which will allow me to be med-free for the first time in 13 years. But thanks to the corruption of the literature, there are no scientific studies that can tell me how much of my original functioning and quality of life I can regain, or if my withdrawal will be difficult. In fact, the only way I can even GUESS at the answers to these questions is by relying on peer-support message boards of patients in similar situations. I think that fact alone speaks volumes of the spectacular betrayal of a patient’s basic rights by psychiatry. And this corruption has been flourishing for decades.
I must remind you that the exposure of a lot of the corruption that you are now aware of is largely the fruits of the labor of the peer recovery movement who have gotten the word out, as well as clear-minded psychiatrists like Dan Carlat and Mickey at 1boringoldman.com, and of course courageous journalists like Robert Whitaker, whose ANATOMY OF AN EPIDEMIC honors evidence-based medicine far better than many of the “studies” sponsored by pharmaceutical companies that formed the core of the biological-based model of psychiatry practiced today. By and large, mainstream psychiatry and the APA couldn’t care less about the corruption and the human rights violations inherent in it (after all, there’s just too much money in it). As long as that continues, psychiatry will continue to spiral into a deep decay of toxic debauchery and a Roman orgy of greed.
If you think I’m exaggerating, spend some quality time over at 1boringoldman.com. Print out as many of his posts as you can (they’re all good), grab a stiff drink (you’ll need it), soak it all in, and just be AMAZED at how far humans can fall when no one is enforcing the rules. And remember it’s been like this since at least 1980 when the DSM-III was introduced.
Finally, if you’d like to hear an hour-long interview I conducted with Robert Whitaker on these subjects and more, go to the link below and download the audio file. The audio is thin mono so headphones are recommended. The interview was posted on survivingantidepressants.org, which is a peer-support message board for those suffering from prolonged SSRI withdrawal syndrome. The administrator of the board, Altostrata, has been suffering with protracted withdrawal for seven years and counting, and she is currently in discussion with researchers about how prevalent this condition is and how overlooked it has been in the literature, which may very well invalidate a large swath of the antidepressant literature.
INTERVIEW LINK: http://www.mediafire.com/?7tpniej544yskx3
If the professionals dont know and are in turmoil where does that leave the patients?
How am I to trust a community that does not trust itself?
With a chronic mental illness and only a high school diploma I dont have the tools and resources to make a well reasoned, educated decision about the treatment prescribed by my care providers. I’m required to trust.
Then when I go online to research the new atypical or ssri or anticonvulsant or benzodiazepine or whatever med my doc picked I find all the anti-psychiatry rhetoric, the horrible personal experience patient blogs/forums, the abstracts for positive and negative studies, the articles trashing the studies or pointing out how horribly designed the studies are or how its all placebo anyway and if I believe in the med it will help me, and all the professional blogs lamenting the corruption of the profession or complaining about not getting paid enough.
But in my 15 min med check I dont have time to ask all the questions I have and my illness is blamed for my basic distrust or my desire to not take a specific med.
It wasnt until my GP and my sleep doc went to bat for me to say that it doesnt matter how helpful the doc thinks a med is, unless it is to directly save my life I can not continue to gain weight. My blood pressure, apnea and diabetes can no longer take it.
I hate to say “get your act together” but I wonder how many professionals are remembering how vulnerable their patient population is?
SG
I appreciate your post a lot. As a person who for years could not find any medication that did not make me crazier than I started out, I can only say I am sorry you are continuing to suffer. I am a shrink because I believe in psychotherapy, which ultimately I had to work at and had to work for me.
While I completely agree with you about pharmaceutical companies and the doctors who cooperate with them and the evil, inhumane shit they pull all for money–from Pfizer with neurontin to Merck with Vioxx, I don’t conclude that psychiatry is any more dead than anything else in medicine. Unlike you I never had faith in corporations or in “fact finding commissions”. I was 13 or so when Reagan locked out the air traffic controllers and began dismantling the unions. So Enron and no bid contracts to the company owned by Cheney’s family for the war Bush started does not surprise me. Compared to that, the fact that there are bad shrinks who collaborate with Pharma does not mean psychiatry is dead. Not every psychiatric medication is bad and not every psychiatrist is bad. It is not that simple.
A LOT of shinks are about to retire. If we are going to change our underpaid, overworked lot in medicine and organize ourselves so that we can advocate for our patients who, generally can not advocate for themselves the next 5 years is our time.
Sideways: Thanks so much for your nuanced and compassionate reply. A quick note: please realize I am suffering BECAUSE of the medication (that I didn’t need to be on in the first place), not because I haven’t found one that works for me.
Now a clarification: I did not say modern psychiatry is “dead” or any more moribund than any other profession. Duane said that. What I was getting at in my post is that we are at an astonishing crossroads in this country and we will have to re-evaluate MANY things (not just psychiatry), and so far I see that re-evaluation of psychiatry occurring not by the psychiatric mainstream like the APA or practicing psychiatrists, but by the “outsiders” like 1boringoldman (a retired psychiatrist) and Robert Whitaker. They are the ones doing the tireless, slogging work of conducting a postmortem on the core literature that laid the framework for the DSM-III era of the bio-medical model of psychiatry. And what they’re finding is largely very, very ugly.
I agree that the next five years may be the proving ground for psychiatry. The generational shift of the “old guard” bio-medical model shrinks leaving the profession can only be a good thing, in my opinion, as is the fact that pharmaceutical companies are pulling out of psychiatry. This will give psychiatry an opportunity to take a long, painful, but desperately needed look at itself and what it’s become over the last 30 years and allow it to HOPEFULLY regroup and FINALLY begin conducting unbiased studies (and some longitudinal unbiased studies, at that!) and not be afraid of what it finds. If psychiatry finds that what Whitaker, Irving Kirsch, 1boringoldman and others are saying is true (mainly, that the meds are often no more effective than placebo for most and that long-term medicating can worsen long-term outcomes), then those results MUST be honored, no matter how painful for psychiatry.
The only way I think psychiatry will be “dead” is if it doesn’t do precisely this. If it continues to practice a model of care that was heavily corrupted from the outset and ignores the growing evidence that it’s highly flawed (and sometimes dangerous), then psychiatry will lose even more favor from the public. BUT if psychiatry does take that long, hard look at the evidence and reconstructs itself — and isn’t afraid of what psychiatry may look like in the future, even if it looks vastly different than what it is today — then it has a chance at a great rebirth.
I must say, however, that it is most encouraging to see a psychiatrist’s blog such as this where he admits his disillusion in his field. This can only be a step in the right direction. Now, if
we just had more psychiatrists doing the work that Whitaker and 1boringoldman are doing, we’d REALLY have something 🙂
My experiences with psychiatry — as a parent of a son with recurring depression/bipolar that started in his mid-teens — have been positive.
We realized early on that there were no “magic bullets,” were not promised any, and knew that it would probably take some time to find the right meds for him. And that’s what happened.
For our family, a caring doctor and Big Pharma (though his meds are all generic now), have allowed our son to get on with his life.
Now, all the people you talked about have the right to their opinions, but they don’t speak for me.
Jackie: I think it’s very important to remember that no matter where we fall on the psychiatric spectrum, we could all benefit from a far more transparent, unbiased, and rigorously scientific evidence base for psychiatry. Even though your experience has been a positive one in psychiatry, it could have easily been the other way around, like Duane’s situation. And vice-versa.
Because of the profoundly tainted evidence-base, one’s outcomes in psychiatry can be more of a lottery than necessary. A better evidence base would serve everyone: it would allow doctors to truly provide informed consent to patients (who are increasingly children) and their parents about both the short and long-term risks, it would provide protocols for people like me on how to safely withdraw from long-term psych med use, and it would ensure that people like your son continue to receive the best care current science has to offer throughout his lifetime IF he decides to stay on medication. As it is currently, very little of this is possible and I’m sure you’d agree that’s a major problem. At the very least, we owe it to this current generation of kids that are coming of age on psych meds to have the best scientific evidence possible on the safety of these medications, and if medications are necessary at all.
And I must also warn you that there is the possibility that the medication(s) your son is on may stop working and may cause disruptive symptoms down the road (maybe even as long as ten years or more down the road). This is similar to my situation. I couldn’t withdraw from my SSRI because of my aforementioned situation, but for many years (close to a decade) they weren’t causing me any side effects so I didn’t worry about it. I too thought that people who talked of long-term damage from drugs were lying. I never thought it would happen to me. But here I am now, where in the last few years I have side effects like pronounced sexual dysfunction and anhedonia that majorly impact my quality of life. I believe a large part of the problem for many is the insidious onset of the side effects, which people chalk up to anything BUT the drug (getting older, stresses in their life, pre-existing medical conditions, etc), and when the side-effects are too strong to ignore or attribute to anything else, it’s been 20 long years on a med and the damage has been done. And with the way things are right now, if you fall in that boat where the meds suddenly turn on you, there’s very little that can be done other than switch horsies on the med merry-go-round to try to regain some kind of equilibrium. I think you’d agree it would be nice to have a strong evidence base of scientifically sound studies to guide you through such a situation, or prevent it from happening entirely.
As an example of evidence-based medicine that can protect patients, below is a link to a story that reports on researcher Nancy Andreasen’s findings that antipsychotic medications can shrink the brain when taken long-term. I don’t mention this article to frighten you or convince you that all meds are bad, but instead to do what so many doctors don’t do: inform you of the long-term risks associated with these medications so you can make an informed risk/benefit decision. I will also admit that these findings are preliminary and the ultimate significance of the findings are still to be determined and need further research. Regardless, if I were a patient about to be treated with these meds, I’d certainly like to know about this study before taking any medication.
Having said all this, it may be hard to believe but I am actually not against the biologically-based model of psychiatry. What I am against is the corrupted evidence-base and the fact that psychiatry has looked the other way for so long at the corruption and continues to practice under the mass delusion that mental illnesses ARE like other biologically-based illnesses (cancer, diabetes, etc) even though there isn’t a shred of evidence in the literature that they are. I’m very much open to the possibility that something like depression or bipolar MAY have a genetic or biological basis (or, maybe after all, IS due to some chemical imbalance!) but we’re certainly not going to discover that if we continue spinning our wheels with the current widespread corruption of psychiatric literature.
And finally, I’d like to say I understand and respect your son’s success with medication. I only recently had it made clear to me that a lot of the talk about psychiatric reform and corruption can be threatening to those who have had GOOD outcomes on meds because they fear that if massive reform happens and the corruption is outed, that somehow their meds will be deemed dangerous and taken away from them. I can very well understand that fear. What I want (and I really believe everyone wants this) is the greatest good for the greatest amount of patients. I deserve to live a full, productive life off meds and access to an evidence-base that allows me to do that, and your son deserves a full, productive life ON meds (if he so chooses), with the added benefit of an improved evidence-base that can maximize his long-term outcome.
And who knows? If studies are done that prove some patients can get well by simply living in assisted-living homes like those of Loren Mosher’s Soteria house, then all the better. Or maybe a combination of exercise, meditation, and nutritional supplements may be all some people need.
The bottom line is a better evidence-base would allow us to use the right tool for the right job. Right now all psychiatry has is a sledge hammer (meds) and we don’t even know how to use the sledge hammer properly. Sure, there are some patients who are lucky enough to need a sledge hammer used in just a certain way and have good outcomes, but for the others who need different tools, well, they’re out of luck. I think you’d agree we as a society can do A LOT better.
Whoops, forgot to add the link: http://www.psychologytoday.com/blog/mad-in-america/201102/andreasen-drops-bombshell-antipsychotics-shrink-the-brain
Sorry for the additional post!
Whoa, that was some reply, with three or four “I think you would agrees …”
No comment on that, but rest assured we are looking out for our son’s best interests, as he gets on with his life.
I read the article. I find 2 problems with using this article on its own as definitive.
1) 211 is a very small sampling
and 2) “In this February report, Andreasen does not tie the drug-related brain shrinkage to an increase in negative symptoms, functional impairment, and cognitive decline. But in earlier articles, she did just that.”
As the author did not go to the Andreasen and ask why this was omoitted in her latest report there is no way to know if she stands by the earlier statements or if she has decided they are no longer true.
Article In Defense of Antidepressants. Thought this was interesting in light of many of the comments.
Of course Kramer will write the opinion letter defending antidepressants being the author of ‘Listening to Prozac’.
On the topic in comments re brain shrinkage on antipsychotics
http://bipolarsoupkitchen-stephany.blogspot.com/2011/02/average-rate-of-gray-matter-loss.html
As some passionately defend their use of their own or loved ones use of pharma antipsychotics or antidepressants, I also passionately speak/write about my daughter’s permanently loss of quality of life and ability to process (think)words, speak, speak in sentences longer than 6 words, care for self, lose friends (all of them) never make it to senior yr or complete high school…. all due to antipsychotic use from age 11 until current (current docs trying to shave down the dose to prevent inevitable withdrawal psychosis that is what always happens to her)of Clozaril.
No one has long term results of use like that, and I hope no one ever does. Anyone using antipsychotics or defending them, go right ahead, the future is wide open to how that will end up. Life, and the quality of it on medications like those are often described by family members as ‘good’ because their loved one is here and with them, but ask the person or observe them, and you might see a less skewed observation… gained weight? dealing with increased depression or annxiety and on benzos or antidepressants? question the drugs, many ppl who have used them and went off retrospectively speak on how they feel the drugs induced those feelings and drug free are lessened.
Rather than look at a study look at the patients in institutions or ones who are worn down and beaten down by the heavy use of the antipsychotics in group homes, these are the silent sufferers not often seen in society and the saddest cases of all. I’ve seen quite a lot in the last decade+ and it’s not a pretty picture. The hundreds of ppl Ive met are worn down by these drugs, and live low quality lives, unable to work, or function as ‘typical’ people in society, now fragile and vulnerable, it’s quite shocking America has not come up with a better plan of action to care for mental health patients. Clearly, the medication based paradigm is not working, if it was the increase of disabled patients wouldn’t be so high and the psych wards would be empty and not full of revolving door patients.
Take a few minutes and watch the vid clip in this post
http://bipolarsoupkitchen-stephany.blogspot.com/2011/05/healing-homes-alternative-swedish-model.html
“Healing Homes, a feature-length documentary film directed by Daniel Mackler, chronicles the work of the Family Care Foundation in Gothenburg, Sweden — a program which, in this era of multi-drug cocktails and psychiatric diagnoses-for-life, helps people recover from psychosis without medication.”
It’s time for America to approach mental illness with alternative thinking for care, people deserve it.
Thanks for this article, Lee. It makes some excellent points and Kramer’s ultimate therapeutic approach — natural modalities primarily and a sparing use of drugs — is sound.
However, I take issue with some of his arguments. Below I’ve run through them, point by point. This was the most logical way to post about this, but obviously it means the post has run on quite long. I recommend printing out the post, as I do with longer posts by others.
-Kramer makes good points that narrow studies may open up possibilities for antidepressant treatment: symptoms such as post-surgical depression, depression from neurological disorders like MS, interferon-induced depression, and post-cardiac surgery depression could all possibly be treated (at least in the short-term) with antidepressants. However, I think he’s a little premature in his claim that “In stroke patients, antidepressants look like a tonic for brain health.” That’s a bold claim, and I would have preferred he mention at least a few more of the articles he emailed to his friends’ neurologists as support for that lofty claim.
I should also mention the placebo response shouldn’t be ruled out even in something as dramatic as regained mobility in stroke patients. It has been documented that Parkinsons patients can have a dramatic reduction of tremors when taking a placebo, for instance. See this link (http://www.pbs.org/saf/1307/video/watchonline.htm) for a segment on a PBS documentary about the placebo effect that directly demonstrates how dramatically Parkinsons patients can “improve” through placebo alone (click on the “expectation pays” video).
There is no mention by Kramer of the possibility that the drugs’ placebo effect may (at least in part) be playing a role in those stroke patients’ recovery. By leaving out this possibility, Kramer is coming close to doing what he says critics of antidepressants are doing: refashioning studies into “editorials with numbers attached.”
-The crux of Kramer’s argument is that the media articles reporting on recent studies that antidepressants are largely no more effective than placebo were largely based on highly flawed and biased studies needs a closer look as well. He speaks very well about how compromised the patient sample really can be in these studies. Unsurprisingly, this “patient group” often looked nothing like real psychiatric patients with real mental illnesses, and it’s not much of a stretch to see how that skewed the outcome data. This is a great point and I’m glad he’s mentioning it as this flaw in pharmaceutical-sponsored drug trials is most grievous.
However, I disagree with some of his points that follow from this central thesis. For one, I honestly can’t agree with his statement that “Nonetheless, the FDA mostly gets it right.” Considering that all the FDA currently requires for drug approval are two successful trials (with an unlimited amount of failed trials) that prove the drug is better than placebo (that is, better than nothing), I’d say that sets the bar pretty low (Unhinged: The Trouble with Psychiatry — A Doctor’s Revelations about a Profession in Crisis. New York: Free Press, 2010. 102-03.). Compounding that is the FDA currently doesn’t require any evidence from drug companies that their new drug is better than any older drug, which has allowed the amount of “me-too” drugs and patent-extenders to balloon in the market. With this in mind, it’s easy to see why there are so many me-too drugs and few novel ones. Patients could certainly benefit from more novel drugs that are the result of rigorous testing, but the FDA has calibrated the drug approval process so that it’s not in the drug companies’ best interests to do such a thing.
This has been proven recently in the mass exodus of pharmaceutical companies from psychiatry. The companies have realized they’ve saturated the market and can only tweak the molecules of existing drugs so much. And, of course, with all the corruption that has come to light recently about those FDA trials, the companies know the pressure — and higher standards for scientific evidence of efficacy — will be on if they try to venture into the territory of new psych medications this time. So they decided to cut their losses and leave psychiatry behind. They didn’t decide to invest long-term in psychiatry by spending R&D money coming up with new drugs and playing fair by not running rigged trials as it wasn’t in their financial interest, and the FDA plays a role in this. The drug companies’ actions speak volumes.
I also take issue with his statement, “Scattered studies suggest that antidepressants bolster confidence or diminish emotional vulnerability — for people with depression but also for healthy people. In the depressed, the decrease in what is called neuroticism seems to protect against further episodes.” Such a statement actually seems to support the evidence that the medication doesn’t actually treat the illness itself since the same response — increased confidence and decreased emotional vulnerability — is consistent across the ill and the well. And I’d like to float the hypothesis that what the patients are experiencing isn’t increased confidence or decreased emotional vulnerability, but merely drug-induced apathy. The APPEARANCE of confidence may indeed follow from a diminished emotional vulnerability, but that emotional vulnerability is diminished simply because the patient is less able to feel the full range of emotions such as fear and anxiety. That is, they’re not confident — they just don’t care. And confidence and apathy are two very different things, even though they appear similar. Confidence (at least in my opinion) is an inner resilience born out of hard-won experience, accomplishments, aptitude, and soul-searching (and, yes, sometimes pure naivete), and apathy is a resignation to life as it is. I should also mention that apathy and decreased emotional response is one of the most common SSRI symptoms, especially in those medicated long-term.
Now, I’m open to the possibility that some of these patients are truly having a “mind-awakening” experience and are not merely numb, but if even some of the patients are really experiencing apathy instead of true confidence, what does that mean for combination therapy of psychiatry and traditional talk therapy? What’s really helping the most out of the two? Is it the med pulling most of the weight? And if it is, is it simply due to apathy and numbness taking the edge off one’s suffering, as a long-term trade-off for real growth that comes through cathartic suffering, which requires full access to strong emotions?
Speaking of long-term, my main issue with Kramer’s article is his support of FDA “maintenance studies.” He says that, “In these trials, researchers take patients who are doing well on medication and switch some to dummy pills. If the drugs are acting as placebos, switching should do nothing. In an analysis that looked at maintenance studies for 4,410 patients with a range of severity levels, antidepressants cut the odds of relapse by 70 percent. These results, rarely referenced in the antidepressant-as-placebo literature, hardly suggest that the usefulness of the drugs is all in patients’ heads.”
I think that Kramer is making the same mistake here that nearly every researcher has in these trials: he’s mistaking relapse for withdrawal. It’s now common knowledge that discontinuation from SSRIs can cause withdrawal. In fact, Eli Lilly sponsored a symposium to address the issue of SSRI withdrawal and researchers Jerrold Rosenbaum and Murizio Fava of Mass General found the rate of withdrawal syndrome to be as high as 80 percent (Stutz, Bruce. “Self-Nonmedication.” The New York Times. May-June 2007.). This figure is eerily close to the 70 percent of “relapse” in the maintenance studies. Co-incidence? Only further study will tell.
But for now, I think it’s safe to assume that a large portion of the literature has been confounded by mistaking withdrawal for relapse, which has many of the same symptomology. It may follow that the patients who went off the drug didn’t become depressed again, but simply that their brains had adapted to the drug and needed it for their brains’ pharmaceutically-induced meta-homeostasis. This has already proven true for other psych meds like benzodiazepines where some patients have persistent cognitive decline and rebound anxiety years after withdrawing from the medication and in antipsychotics which can cause permanent brain remodeling causing side effects like tardive dyskinesia. The time has come to ask if something similar could happen with SSRIs, and the longer we mistake withdrawal for relapse, the longer we have a reason to keep patients on meds long-term and thus increasing their risk for persistent side effects and very difficult withdrawals.
Robert Whitaker has recently been investigating this: here is the link to his new blog post on “tardive dysphoria”: http://madinamerica.com/madinamerica.com/Whitaker.html I should also mention that emerging literature on PSSD (Post-SSRI-Sexual-Dysfunction), a condition where sexual dysfunction can last for years or even seemingly indefinitely after SSRI discontinuation, speaks to some kind of persistent brain remodeling similar to benzos and antipsychotics. Finally, I should mention that withdrawal symptoms may not immediately appear in some patients. I have read many anecdotal stories on websites where withdrawal did not surface a month or even more after being off the SSRIs. And the symptomology was consistent with discontinuation syndrome (brain zaps, insomnia, crying spells not experienced when previously depressed, and various autonomic system dysfunction). I recently met a woman who didn’t experience withdrawal until 6 months after her last Paxil dose, and her withdrawal lasted for three years.
-I find fault with Kramer’s statement, “Antidepressants have something like celebrity status, exposing them makes headlines.” I’d argue that psychiatry itself (the APA, NIMH, and powerful mainstream psychiatrists) set themselves up for this by purposefully elevating the meds to celebrity status. This “celebrity status” that antidepressants have enjoyed is largely the orchestration of a sustained media blitz conducted by psychiatry unparalleled in modern medicine, beginning with the publication of the DSM III in 1980. Just a few examples from the “The Rise of an Ideology” chapter of Whitaker’s ANATOMY OF AN EPIDEMIC:
-“In 1981, the APA established a ‘division of publications and marketing’ to ‘deepen the medical identification of psychiatrists,’ and in very short order, the APA transformed itself into a very effective marketing machine.”
-Examples of this “marketing machine” were the APA establishing its own press in 1981, establishing a “public affairs institute” to provide media training for high-profile “experts” to speak to the media about the new medications (cue the APA-led workshops with titles like “How to Survive a Television Interview,” of which there were 9 in 1985 alone), and handing out awards to journalists whose work it liked. Soon APA spokepersons were on major shows like Phil Donahue, tantalizing audiences of the revolutions soon to come in psychiatry.
This media blitz helped soften the mark (the mark being the media and the general public) so when Prozac appeared, the media was salivating and all-too-willing to believe the biased trials. And the NIMH got in on it too with their Depression, Awareness, Recognition and Treatment program (DART).
So, if I may be so bold, I don’t think the righteous ribbing of antidepressants in the press is unfounded. It’s only natural the public feels ripped off when developments like those above have come to light. Psychiatry chose to market the drugs in this way and collude with pharmaceutical companies, and it’s in the best interest of patients and psychiatrists everywhere that we get to the bottom of this.
Finally, a few more points that Kramer makes:
-I agree that washout trials hold promise for better research and they should be used more often. I also agree that Dr. DeRubeis’s research was suspect and speaks to his bias as a psychotherapist.
-I wholeheartedly agree with Kramer that “better-designed research may tell us whether there is a point on the continuum of mood disorder where antidepressants cease to work.”
-I also agree that antidepressants have “earned their place in the doctor’s satchel,” with the condition that now the task laid before us is to take a hard look at the data and conduct unbiased (and longitudinal studies) to determine just how large a place it should claim in the satchel.
SG:
I appreciate your perspective, insight and relevant references. Do you blog/publish elsewhere?
Stephany:
Your experience is troubling. Thank you for sharing it and for your passion in advocating for safe and effective care.
My family was horrifically damaged by psychiatric drugs making illness far worse. How do I know this, a literal miricle occurred when proper treatment was found—low doses of lithium.
You talk about psychiatry being damaged as a profession, I hear nothing about patients being damaged. What does a charming, mentally healty young person say to a prospective employer———-it was all a big mistake, they gave me anti depressants instead of mood stabilizer mono therapy. I got worse but I thought it was the disease.
Addendum: One may indeed, and should indeed sometimes put an atypical into the brain of a patient, with the pateint’s consent. Anyone who does so without a lot of fear has an ethical problem. We just don’t know what these things are doing.
I am really impressed with your writing skills as well as
with the layout on your blog. Is this a paid theme or did you modify it yourself?
Anyway keep up the nice quality writing, it’s rare to see a great blog like this one these days.