 You’ve probably noticed widespread TV advertisements lately for Cymbalta, Eli Lilly’s blockbuster antidepressant. However, these ads say nothing about depression. Sure, some of the actors may look a little depressed (the guy at right, from the Cymbalta web site, sure looks bummed), but the ads are instead promoting Cymbalta for the treatment of chronic musculoskeletal pain, an indication that Cymbalta received in August 2010, strengthening Cymbalta’s position as the “Swiss Army knife” of psychiatric meds. (I guess that makes Seroquel the “blunt hammer” of psych meds?)
You’ve probably noticed widespread TV advertisements lately for Cymbalta, Eli Lilly’s blockbuster antidepressant. However, these ads say nothing about depression. Sure, some of the actors may look a little depressed (the guy at right, from the Cymbalta web site, sure looks bummed), but the ads are instead promoting Cymbalta for the treatment of chronic musculoskeletal pain, an indication that Cymbalta received in August 2010, strengthening Cymbalta’s position as the “Swiss Army knife” of psychiatric meds. (I guess that makes Seroquel the “blunt hammer” of psych meds?)
Cymbalta (duloxetine) had already been approved for diabetic neuropathy and fibromyalgia, two other pain syndromes. It’s a “dual-action” agent, i.e., an inhibitor of the reuptake of serotonin and norepinephrine. Other SNRIs include Effexor, Pristiq, and Savella. Of these, only Savella has a pain [fibromyalgia] indication.
When you consider how common the complaint of “pain” is, this approval is a potential gold mine for Eli Lilly. Moreover, the vagueness of this complaint is also something they will likely capitalize upon. To be sure, there are distinct types of pain—e.g., neuropathic, visceral, musculoskeletal—and a proper pain workup can determine the exact nature of pain and guide the treatment accordingly. But in reality, overworked primary clinicians (not to mention psychiatrists, for whom hearing the word “pain” is often the extent of the physical exam) often hear the “pain” complaint and prescribe something the patient says they haven’t tried yet. Cymbalta is looking to capture part of that market.
 The analgesic mechanism of Cymbalta is (as with much in psychiatry) unknown. Some have argued it works by relieving the depression and anxiety experienced by patients in pain. It has also been proposed that it activates “descending” pathways from the brain, helping to dampen “ascending” pain signals from the body. It might also block NMDA receptors or sodium channels or enhance the body’s own endorphin system. (Click on the figure above for other potential mechanisms, from a recent article by Dharmshaktu et al., 2011.)
The analgesic mechanism of Cymbalta is (as with much in psychiatry) unknown. Some have argued it works by relieving the depression and anxiety experienced by patients in pain. It has also been proposed that it activates “descending” pathways from the brain, helping to dampen “ascending” pain signals from the body. It might also block NMDA receptors or sodium channels or enhance the body’s own endorphin system. (Click on the figure above for other potential mechanisms, from a recent article by Dharmshaktu et al., 2011.)
But the more important question is: does it work? There does seem to be some decent evidence for Cymbalta’s effect in fibromyalgia and diabetic neuropathy in several outcome measures, and in a variety of 12-week trials summarized in a recent Cochrane review.
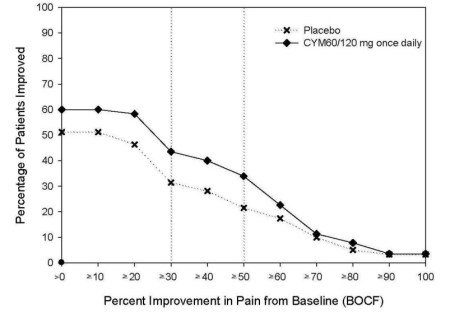 The evidence for musculoskeletal pain is less convincing. In order to obtain approval, Lilly performed two studies of Cymbalta in osteoarthritis (OA) and three studies in chronic low back pain (CLBP). All CLBP studies showed benefit in “24-hour pain severity” but only one of the OA studies showed improvement. The effects were not tremendous, even though they were statistically significant (see example above, click to enlarge). The FDA panel expressed concern “regarding the homogeneity of the study population and the heterogeneity of CLBP presenting to physicians in clinical practice.” In fact, the advisory committee’s enthusiasm for the expanded indication was somewhat muted:
The evidence for musculoskeletal pain is less convincing. In order to obtain approval, Lilly performed two studies of Cymbalta in osteoarthritis (OA) and three studies in chronic low back pain (CLBP). All CLBP studies showed benefit in “24-hour pain severity” but only one of the OA studies showed improvement. The effects were not tremendous, even though they were statistically significant (see example above, click to enlarge). The FDA panel expressed concern “regarding the homogeneity of the study population and the heterogeneity of CLBP presenting to physicians in clinical practice.” In fact, the advisory committee’s enthusiasm for the expanded indication was somewhat muted:
Even though the committee also complained of the “paucity of sound data regarding the pharmacological mechanisms of many analgesic drugs … and the paucity of sound data regarding the underlying pathophysiology,” they ultimately voted to approve Cymbalta for “as broad an indication as possible,” in order for “the well-informed prescriber [to] have the option of trying out an analgesic product approved for one painful condition in a patient with a similar painful condition.”
 Incidentally, they essentially ignored the equivocal results in the OA trials, reasoning instead that it was OK to “extrapolate the finding [of efficacy in CLBP] to other similar musculoskeletal conditions.”
Incidentally, they essentially ignored the equivocal results in the OA trials, reasoning instead that it was OK to “extrapolate the finding [of efficacy in CLBP] to other similar musculoskeletal conditions.”
In other words, it sounds like the FDA really wanted to get Cymbalta in the hands of more patients and more doctors.
As much as I dislike the practice of prescribing drugs simply because they’re available and they might work, the truth of the matter is, this is surely how Cymbalta will be used. (In reality, it explains a lot of what we do in psychiatry, unfortunately.) But pain is a complex entity. We have to be certain not to jump to conclusions—like we frequently do in psychiatry—when/if we see a “success story” with Cymbalta.
To the body, 60 mg of duloxetine is 60 mg of duloxetine, whether it’s being ingested for depression or for pain. If a patient’s fibromyalgia or low back pain is miraculously “cured” by Cymbalta, there’s no a priori reason to think that it’s doing anything different in that person than what it does in a depressed patient (even though that is entirely conceivable). The same mechanism might be involved in both.
The same can be said for some other medications with multiple indications. For example, we can’t necessarily posit alternate mechanisms for Abilify in a bipolar patient versus Abilify in a patient with schizophrenia. At roughly equivalent doses, its efficacy in the two conditions might be better explained by a biochemical similarity between the two conditions. (Or maybe everything really is bipolar! —sorry, my apologies to Hagop Akiskal.)
Or maybe the medication is not the important thing. Maybe the patient’s perceived need for the medication matters more than the medication itself, and 60 mg of duloxetine for pain truly is different from 60 mg duloxetine for depression. However, if our explanations rely on perceptions and not biology, we’re entering the territory of the placebo effect, in which case we’re better off skipping duloxetine (and its side effect profile and high cost), and just using an actual placebo.
 Bottom line: We tend to lock ourselves into what we think we know about the biology of the condition we’re treating, whether pain, depression, schizophrenia, ADHD, or whatever. When we have medications with multiple indications, we often infer that the medication must work differently in each condition. Unless the doses are radically different (e.g., doxepin for sleep vs depression), this isn’t necessarily true. In fact, it may be more parsimonious to say that disorders are more fundamentally alike than they are different, or that our drugs are being used for their placebo effect.
Bottom line: We tend to lock ourselves into what we think we know about the biology of the condition we’re treating, whether pain, depression, schizophrenia, ADHD, or whatever. When we have medications with multiple indications, we often infer that the medication must work differently in each condition. Unless the doses are radically different (e.g., doxepin for sleep vs depression), this isn’t necessarily true. In fact, it may be more parsimonious to say that disorders are more fundamentally alike than they are different, or that our drugs are being used for their placebo effect.
We can now add chronic pain to the long list of conditions responsive to psychoactive drugs. Perhaps it’s also time to start looking at pain disorders as variants of psychiatric disorders, or treating pain complaints as symptoms of mental disorders. Cymbalta’s foray into this field may be the first attempt to bridge this gap.
Addendum: I had started this article before reading the PNAS article on antidepressants and NSAIDs, which I blogged about earlier this week. If the article’s conclusion (namely, that antidepressants lose their efficacy when given with pain relievers) is correct, this could have implications for Cymbalta’s use in chronic pain. Since chronic pain patients will most likely be taking regular analgesic medications in addition to Cymbalta, the efficacy of Cymbalta might be diminished. It will be interesting to see how this plays out.


Wow. I never knew that medications such as Cymbalta could be released without hard evidence that it would improve back pain or whatever it is claiming. Quite a scary thought really. It was interesting that the same drug is used for psychological treatment too. I think placebo effect definitely plays a large role in its effectiveness in that area. It seems strange that one drug could target such different things. Definitely learnt something from your post today, cheers!
If this were true only of psychoactive meds, that there is the chicken and the egg quandry, “pain disorders as variants of psychiatric disorders, or treating pain complaints as symptoms of mental disorders. ” it would make sense. As a psychiatrist I understand why you would look at it with only the 2 options but you neglect other meds used for other reasons but have an effect on pain, such as anticonvulsants . Tegretol, for instance, is for seizure disorder but also works on trigeminal neuralgia, a definite pain complaint and pain disorder, while one dosage form, Equetro, has been approved for treating bipolar disorder.* Does it then follow that trigeminal neuralgia or seizures are really psychiatric disorders ? (The same question can be asked re Lamictal and neurontin)
*http://www.medicinenet.com/carbamazepine/article.htm
I find it too easy that too many physicians, based on their blogs/posts want to classify chronic pain as a psychiatric illness. It would be easier, in the short run, to do that, easier for the docs not the patients who get the label of psychiatric but no help for the physical pain.
(And this is not to say that depression is not an issue for many with CIP. Lliving in chronic intractable pain can cause depression. And I do not discount that depression can result in physical complaints, one of them possibly being chronic pain.)
Carol Jay Levy
author A PAINED LIFE, a chronic pain journey
http://womeninpainawareness.ning.com/
http://apainedlife.blogspot.com/
Carol,
Thanks for your thoughtful comment. Unlike many of my posts, this one was not meant to be “practical”– i.e., what should we “label” these conditions, what medications should/shouldn’t we use for these disorders, which specialty (neurology, psychiatry, anesthesia, etc) should treat these conditions, etc.
Instead, I simply wanted to reflect that the boundaries we draw between physical & mental conditions are very vague indeed. (Of course, many of us have known that for a while.) When we start using a “psychotropic” medication for a “physical” ailment– if it works, that is– we should think of it as treating the entire person, rather than a discrete set of symptoms.
It’s like the patient who comes in and says he’s taking “Neurontin for my anxiety, Lamictal for my seizures, Cymbalta for my depression, Elavil and oxycodone for my pain, and Wellbutrin to stop smoking.” (Yes, this happens. A lot.) The body isn’t compartmentalized that way, even though our professional boundaries, drug classes, and textbook chapters are.
Hi Steve,
Yes treating the whole person would be nice. I find many pain patients do get treated symptom by symptom, body part by body part. (And I have rarely had a visit with a GP or specialist where thay have asked about issues other than the complaint for which I made the appointment.
Its interesting, with your example, absent the oxycodone, the rest all have separate and distinct actions for other disorders than the one for which the patient has (or believes them to have been) prescribed.
I don’t know any psychiatrists that “lock” themselves into the biology of what they’re treating, or think that Cymbalta, or other SNRIs, SSRIs, DNRI, are inherently “antidepressants.”
When you prescribe fluoxetine, you shouldn’t think, “I’m giving an antidepressant”, rather than I’m giving an anti-anxiety/PTSD/impulsivity reducer that also is sometimes used for depression. Or, any combination of that? If someone thinks that “fluoxetine” has an inherent anti-depressant mechanism, this is truly concerning.
What inherent quality of a medication let’s us know prior to a trial that the medication is an “antidepressant”?
Diphenhhydramine has more serotonin reuptake than mirtazapine, and mirtazapine has more selective histamine blocking than diphenhydramine, yet some think, “I’m prescribing an “antihistamine” or an “antidepressant” respectively.
I want to add, too, that the primary theories of the biology of mental illness are based on response to medications. Once you realize that fluoxetine is an “anxiolytic” sometimes used for depression, you stop making assumptions that depression results from serotinin deficiency/abnormalities.
No, wait! Fluoxetine is an “anti-premature ejaculationist”, therefore premature ejaculation is caused by serotonin deficiency.
Any psychiatrist “locked” into the biology has absolutely no idea what they’re doing.
Gary has it all backwards. When a patient’s symptoms respond to fluoxetine, you finally know the patient was suffering from fluoxetine-responsive disorder. These discussions suffer from the limitations of our classification of illness and drug. I wouldn’t worry about whether we classify chronic pain as a psychiatric disorder. Chronic pain is chronic pain. All in your head? Maybe not, but a lot of it is.
What exactly is backwards? Everything written is precisely true. Which sentence is backwards?
By the way, you’re comment is seriously flawed. When they respond to fluoxetine, it’s almost statistically equally likely that they’re responding to placebo. You are factually, objectively incorrect in the interpretations you are making, and, frankly, I hope you are not a physician.
Fill in this blank
This phrase/sentence is backward: _________________________ .
Movie doc you wouldn’t worry but those of us with chronic intractable pain have had our fill of being told it is psychiatric despite indications to the contrary. Unfortunately it still stigmatizes patients when they have a diagnosis of psychiatric disorder. It also denies the body (i.e. not in your head) part of the disorder, which for many in CIP is most if not all of it.
That being said it took me years to stop getting upset when I was told the pain was “all in my head” What I heard was the subtext of psychiatric disorder. What the truth was, it WAS all in my head, I have trigeminal neuralgia, atypical facial pain and anaesthesia dolorosa, the first 2 secondary to a partial sturge-weber.
I am not a medical person but I agree that a lot of the pain may be in our heads. My theory is that the brain remembers the pain, continues with that neural memory response, and then may be unable to let go of that pain memory; and the body responds accordingly. It seems to me that this may be the reason, for instance, one has anaesthesia dolorosa in an area that is, for all intents and purposes, numb (or absent a limb altogether.)
Lighten up, Gary, my “backwards” statement was facetious. I was basically agreeing with you, and unfortunately for all of us, (especially me) I am a physician.
And leejcarol, I was trying to agree with you. We need to destigmatize “all in your head.” You also mention an association of CIP with “depression.” We hear that all the time from non-psychiatrists who claim they can’t find a physical basis for pain. What I see is not that CIP patients necessarily have a mood disorder distinct from their pain, but that even acute pain symptoms, but especially chronic pain symptoms, overlap with symptoms of depressive disorders. For example, it’s not really accurate to say that someone who retreats from usual activities while in pain has lost interest in quite the same way as someone in a Major Depressive Episode. I have seen patients with physical injuries who endured numerous failed attempts to treat “depression” miraculously lose the depression when the physical pain resolved. The pain didn’t cause depression, it just looked like depression. And depression definitely didn’t “cause” the pain or the response to pain.
“I wouldn’t worry about whether we classify chronic pain as a psychiatric disorder. Chronic pain is chronic pain. All in your head? Maybe not, but a lot of it is.”
That is the kind of sentence that tends to get us riled up, because it sounds as though it should be a psych dx. But give someone a psych dx and that is often the end of other doctors taking their complaints of pain seriously.
I remember when I was in a pain clinic, in 1980. One patient had bodywide pain and occasional loss of bowel and bladder control. This started after a statue fell on her foot. She was repeatedly pigeonholed as having psych disorder, Afterall what kind of story is this, something falls on her foot and her whole body becomes pained? She must be in a clinical depression with a lot of somatization, a malingerer, or be suffering from other mental disorder. If a doctor were to examine her today the diagnosis would be clear. She has RSD (CRPS). The psych diagnosis was the way of saying “I don’t know what is wrong with her body therefore it must be psychiatric.”
One other quick anecdote. I had hx of non clinical depression. I developed severe pain in my arm and pulse disappeared when I turned my head. A neurologist decided, despite the outright physical and textbook symptoms of scalenus anticus syndrome but knowing I had this depression hx, that the pain was from depression. He told the surgeon he should not operate on me because it was a psych issue. Thankfully the surgeon did not listen. There was a juxtaposition of vessels, removal of the rib and resection immediately offered relief. For the above woman and myself, a psych dx kept her in continued suffereing and absent a thoughtful surgeon, would have done the same for me.
I was prescribed Cymbalta for depression, and was taking the drug for about a year. I decided the negative side effects out weighed the positive, and opted to stop taking the drug. I’ve been on Zoloft and Effexor, and coming off those medications involved about 2-3 weeks of weaning myself off. Cymbalta took about 6 months to fully come off the drug without severe nausea, dizzyness and such side effects. The withdrawal was far worse than any other drug I’d been on, which was alarming considering I found Zoloft to be the most “sedating”.
Here’s how well Cymbalta treats pain.
These polls of patients show:
– Cymbalta dead last among 85 treatments for fibromyalgia http://curetogether.com/blog/2011/08/10/patients-say-fibromyalgia-drugs-make-things-worse-rest-is-best/
– Cymbalta dead last among 35 treatments for neuropathy http://curetogether.com/blog/2011/08/16/neuropathy-study-results-800-people-rate-35-treatments/
– Cymbalta (and Wellbutrin) very mediocre among 83 treatments for depression (Effexor and Paxil barely effective) http://curetogether.com/blog/2011/05/03/23-surprisingly-effective-treatments-for-depression-one-year-later/ — exercise, pets, art therapy, talk therapy rate much higher.
Perhaps it would benefit all, patients and clinicians alike, if pain could be approached more open-endedly, acknowledging the vast amount of what is yet unknown and refraining from trying to find an uncomplicated answer for a “chicken-or-the-egg” type query. Pain is sometimes the causitive, exacerbated by new onset or existing but not yet problematic psychiatric issue(s), unexpected life-events (I once had a patient comment it was an inconvenient time for her to get cancer???) or any of a variety of sequences. Speaking as an indivdual who experienced all of these, some in multiples and as a clinician who has seen a lot of these “sequences” as well as how the individuals differ in their abilities to cope with some or all of it, we need to find what works for each patient and recognize the complexity of that ugly four letter word. And, an aside, the organization I practice with does not include cymbalta in its current formulary so my first encounter with it, I could not, after looking it up on the trusty Lexicomp, figure out why the patient was taking it-no symptoms.diagnosis matched the indications-the patient told me it was prescribed for incontinence. Didn’t see that mentioned so far so I thought I would include it as a bit of pharmacological trivia. I must also add that most GPs today are alotted a 15 minute window to meet, assess, and effectively treat each patient. God help them if they haven’t read the latest journal, can’t read between the lines, the patient forgets to mention that insignificant CARDINAL symptom-“oh, I’ve had that forever, that’s not why I’m here”-, or they left their crystal ball at home. We need to stop being cynical (no I’m not a new grad), be mindful and open, and not stop working together to find the best answer. Thank you to all of you who aren’t giving up.
Tamara McCauley, RN, chronic pain patient
I had a MVA, head-on, almost, just had time to veer a little to the left. Pain in neck since then on my right C5-7. Driver did accelerate thinking “it’s clear” and found 100% at fault. Airbags deployed. Pain since, over four years, in my hands, arms & moved to little toes. Huge bruise on breast. Now need to get debris removed from that. Bladder went south. Pelvis adjusted by chiropractic after unsuccessful “bladder therapy” that only addressed kegeling by the million and trying to lift muscles that had no support from pelvis. Diagnosed with CRPS after about 8 weeks. Pain specialist diagnosed with RSD. Several neck epidurals and one SGB later, some doctors after that said I have it, and some, I don’t. First doctor recanted. Some said neurontin & Lyrica, but I wait and bite my pain, worse at night. Jekyll & Hide. Finally, saw world famous specialist that confirmed diagnosis of RSD/CRPS. Tried gabapentin. Quit after two weeks because I almost killed someone in a parking lot who went by my car; not seeing him. Now another locale doctor said, I don’t have it, again back to square one. Wants to put me on Cymbalta. My conclusion: there is no pain killer for pain that is neuropathic. All drugs have other uses first. I don’t want drugs for epilepsy or depression that “maybe” help me with my pain, but give me side effects that make my pain look less. Chronic pain is now my friend. I rather keep my brain intact than sacrifice it to side effects for drugs that have been developed for other diseases. Unless there is a drug exactlyfor what I have and proven to help, I will not go on any. Now they don’t like that!!!! But I don’t care. Love mornings, hate night. But at least I have some normal time left. Good Night!
Adriana, each of us has to decide which is worse – thepain or the side effects of the drugs. For me it was the patter. I tried tegretol (the first line anticonvulsant for trigeminal neuralgia) 4 times, the 1st time, loss of balance, spatial hallucinations, difficulty talking and thinking and no benefit. For some reason I agree to try it 3 more times and on the 4th it worked complately with no side effects. (I did have to stop after long time because of a bad white blood count, not necessarily related but also a potential risk from the med.)
I tried Cymbalta for maybe a day and could not tolerate the side effects. As someone with neuropathy I am tempted to consider trying it again.
CIP has no commonality, at this point, RSD different from Rheumatoid arthritis, form Ms, etc. (ironic ad for lyrica for pain just came on – I also tried that with awful side effects). There is no med that will be specific. Although off point somewhat we need to have a concensus on the basis cause of CIP, such as neuropathy. Then we willk be better able to have drugs that are not shatter shot.
Hello there, I’ve been taking Cymbalta 60 mg for 6 years or so, (I’m 42, other wise in good health) in the last month arthritis like pain is back only more intense and in more body parts. My Dr wants me to double the dose, I guess I will, the pain is debilitating. My concern is: am I masking something else maybe bigger with Cymbalta?
Your input would be greatly appreciated
Gracias 🙂
I’m truly getting the design and layout of your site. It’s
a very easy on the eyes which makes it much more
enjoyable for me to come here and visit more often. Did you hire out a developer
to create your theme? Fantastic work!
I have had lower back pain for many years. MRI’s showed a slow increase in a herniated disc between L4/L5. As the back spasm episodes became more frequent (in bed for days unable to walk) I saw orthopedic surgeons, nuerosurgeons, sports medicine, chiropractor, accupuncture, etc. Latest MRI showed a 7ml extrusion spread both left and right. Close the to the threshold of needing a microdischectomy (Tiger Woods surgery). The constant pain led to depression and anxiety and I sought a pyschiatrist who prescribed 20mg Cymbalta. After two weeks my pain subsided and I felt better than I had after edidural steroid injections in my back. Although I still have no back strength and overstraining my back will still put me in bed, I have had a relatively pain free year. I’m sure my MRI would show a 9ml etrusion by now and I still have that option but so far the Cymbalta has been a miracle.
I’ve been on cymbalta for 7 months and it does nothing for back pain… Just a Nausicaa feeling for 12 hours and tons of sweating……thanks Eli Lilly for nothing your product sucks…. It’s bad when you have to go to the streets to buy meds that work………